
One of the most unpleasant skin diseases is ringworm. Depending on the degree of damage, two categories of diseases are distinguished: dermatomycosis and onychomycosis. In the first case, the skin is affected, and in the second, the nails. To successfully get rid of harmful microorganisms, you need to know what foot fungus looks like and how to fight it.
Main types
Specialists in the field of dermatology identify several types of fungus on the feet, which differ from each other in the nature of the impact and the causative agent. As for pathogenic microorganisms that cause the development of fungal diseases, they can be:
- musty;
- yeast;
- dermatophytes.
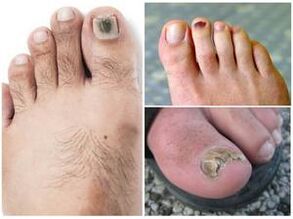
Exposure to these parasites leads to the development of a dangerous disease called rubromycosis, which involves the skin of the feet. Additionally, the disease can vary in clinical manifestations and may be membrane-like, moccasin-like, or vesicular.
The development of the fungus causes excessive saturation of blood vessels, dryness and peeling of the skin. Furthermore, the process itself is slow and without significant symptoms. The first sensations of itching or burning are felt only after a serious injury to the foot. The nail deformation process soon begins, resulting in blisters, crusts, plaques and pustules.
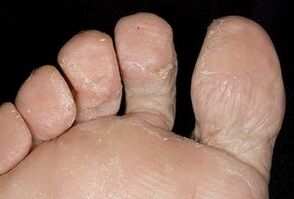
If the necessary measures are not taken, the scale of damage will be colossal and the process of walking will be accompanied by pain. Knowing what foot fungus looks like and how it manifests itself, the patient can seek help from a specialist in time and avoid dangerous consequences.
When it comes to therapeutic treatment, it is important to know the types of disease. The method of approaching the problem is determined only after a comprehensive examination under a microscope and drawing up a clinical picture. Various exfoliating products are used to clear up rashes. These include ointments and creams containing salicylic acid. Complex treatment also includes antifungal medications.
If the degree of damage is very serious, highly effective compresses and emollients are used. Success in combating the disease depends on the patient's responsibility and their willingness to start treatment on time.
Infection methods
There are many reasons and factors that determine nail damage caused by fungal diseases. In most cases, this happens directly - when the nail plates come into contact with the ground or vegetation, sick people or animals. As for the indirect paths, they look like this:
- If a person uses objects and personal belongings of a fungus carrier.
- If a person comes into contact with things intended for caring for a pet.
There are also many predetermining factors that increase the risk of developing ringworm. This includes age-related features, since young children are much more likely to suffer from the disease due to excessively thin skin and a lack of necessary protective functions in the body. 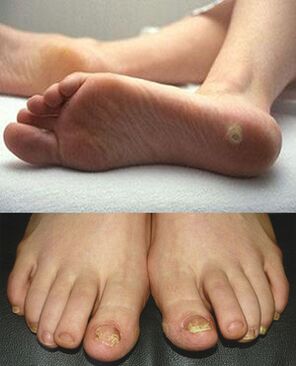
Furthermore, a fungal infection attacks a patient with a deteriorated immune status. If the immune system is weakened, it cannot fight such manifestations, which leads to destructive processes.
Other factors include:
- Insufficient functioning of the nervous and endocrine systems. Because of this, protective mechanisms are weakened.
- The development of chronic infectious diseases that negatively affect the immune system, increasing the likelihood of fungal development.
- Excessive foot sweating. This discomfort is a congenital pathology or the result of wearing uncomfortable shoes.
- Changes in the composition of sweat. This process creates a fertile ground for fungal microorganisms, which leads to their activation.
Symptoms of rubrophytosis
A parasite called Tr. Mentagrophytesvar is the main causative agent of the dangerous fungal disease rubrophytosis. Due to its small size, it instantly settles in the stratum corneum or granular layers of the skin, causing the development of allergies and other unpleasant processes. In most cases, the vital activity of the parasite is accompanied by the following reactions:
- Swelling with dense crust.
- The appearance of pustules and swelling.
- Severe skin corrosion.
- Appearance of scales and crusts on the skin, causing pain.
- Yellowing and deformation processes of the nail plates.
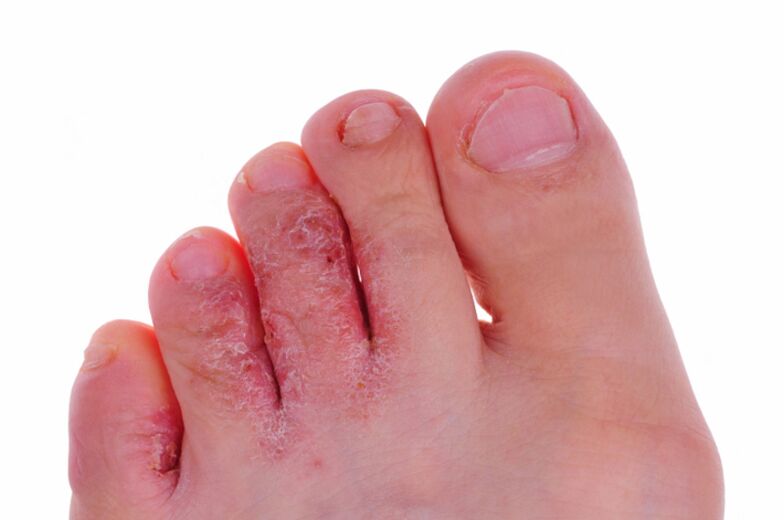
In addition, severe itching and the development of pain when walking cannot be ruled out. During the clinical examination, the specialist draws a general picture and describes the symptoms when examining the scraper.
If the disease progresses rapidly and worsens, the patient may be prescribed silver nitrate 0. 25%, resorcinol 1% and calcium 10%. Antihistamines are used to combat allergic manifestations. In severe cases, highly effective antifungal medications combat the symptoms of rubrophytosis.
Candidiasis of the foot
Foot candidiasis is rare. The causative agent of the disease are dangerous fungi of the genus Candida, which exist peacefully in any organism, but are conditionally dangerous and do not pose a great threat. But if the number of microorganisms starts to increase, it will cause discomfort and serious health consequences. Additional factors contribute to this, including deterioration of the immune system, frequent hypothermia, stressful situations and an unhealthy lifestyle. As for external factors, these include:
- Prolonged exposure to water causes massive separation of skin layers from each other.
- Accidents at home or at work.
- Wearing shoes of the wrong size or material.
Manifestations of onychomycosis
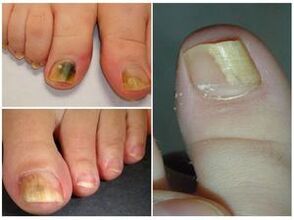
When trying to find out what the fungus on the toes looks like, you need to learn about another dangerous type of pathology - onychomycosis. Its development is accompanied by fungal nail infection after water procedures in common swimming pools, showers and saunas. In terms of prevalence, the disease is not inferior to ringworm, since scales with dangerous parasites quickly separate from the nail plates and are found on the surfaces of fabrics, benches or carpets. If there is a lot of humidity in the environment, the parasite not only finds itself in comfortable conditions, but also begins to work on reproducing the colony.
In the initial stages, the pathogen affects the skin of the feet, causing an itching sensation. As a result, the patient feels like scratching their foot, but this only makes the problem worse. Soon the skin becomes covered with small cracks and scratches, and pathogens begin to settle under the nail and actively multiply.
The likelihood of encountering pathology increases many times over with nail injuries, unbalanced blood circulation and the presence of complex diseases, including diabetes and sexually transmitted diseases.
Depending on the form and degree of damage, nail fungus is divided into three groups:
- Normotrophic. As it develops, the nail color becomes yellowish-brown. The thickness and shape of the nail remain the same.
- Hypertrophic. This causes a final change in color, loss of shine and deformation of the nail shape. This type of onychomycosis causes pain and does not allow the patient to move freely. The problem can be made worse by wearing uncomfortable shoes.
- Onycholytic. The pathology leads to a change in the shade of the nails, causing them to turn brown. Furthermore, the boards lose their usual strength and begin to delaminate. Deformed layers appear on exposed areas of the nail bed.
Effective treatment

To treat the disease, the use of local antifungal drugs is practically useless, which is explained by the deep penetration of microorganisms under the nails. Before starting to combat the pathology, it is necessary to locate the fungus. To do this, specialists prescribe keratolytic medications or patches to the patient. Sometimes the problem is solved mechanically, cutting out deformed and dead areas of the nail plate with a special file or tweezers. When carrying out this procedure, it is necessary to make sure that the instrument is clean.
The most effective way to combat nail fungus is the combined use of stickers and mechanical nail cleaning. As a keratolytic agent, you can use a set consisting of a sticker, a nail file and a special ointment. At the end of the nail removal procedure, it is necessary to use systemic antifungals.
Folk remedies

It is quite possible to get rid of fungal infections on your feet without the help of a specialist. However, self-medication must be treated with special responsibility, understanding that such a process can require a lot of time and effort. It is also necessary to take into account that different mushrooms react in their own way to the action of any medicines or folk remedies. Home medicine, if used incorrectly, can only worsen the problem by helping to detect parasites.
To prevent such a development of events and successfully destroy the fungal colony, it is necessary to combine proper cleansing of the skin with cleansing the body of pathogenic microorganisms and comprehensive restoration of the epidermal layer. To do this, it is advisable to take baths and clean your feet and palms daily with antiseptics. The most effective folk remedies for baths are:
- Boric acid;
- Apple vinegar;
- hydrogen peroxide.
To prepare a bath, you need to take 20 grams of one of the above compounds and dilute it in a liter of boiled water. After that, the feet are placed in the solution for 20 to 40 minutes. To notice a significant improvement in the condition of your nails, it is enough to carry out these procedures regularly for several weeks.
To cleanse the skin of redness, itching and burning, it is recommended to wipe your feet daily with a mixture of soda with added salt. A good antibacterial and anti-inflammatory scrub can be a mixture of equal amounts of minerals and essential oils. The selected components are mixed and the affected areas are covered with the finished mixture.
Tar soap is a serious enemy of fungi. Contains birch tar, which has long been considered one of the most powerful antibacterial substances. It must be applied to the affected areas and washed off after 5 minutes. Treatment with this soap lasts two weeks. At the end of the procedure, the skin is treated with zinc cream or ointment.
Hardware Solutions
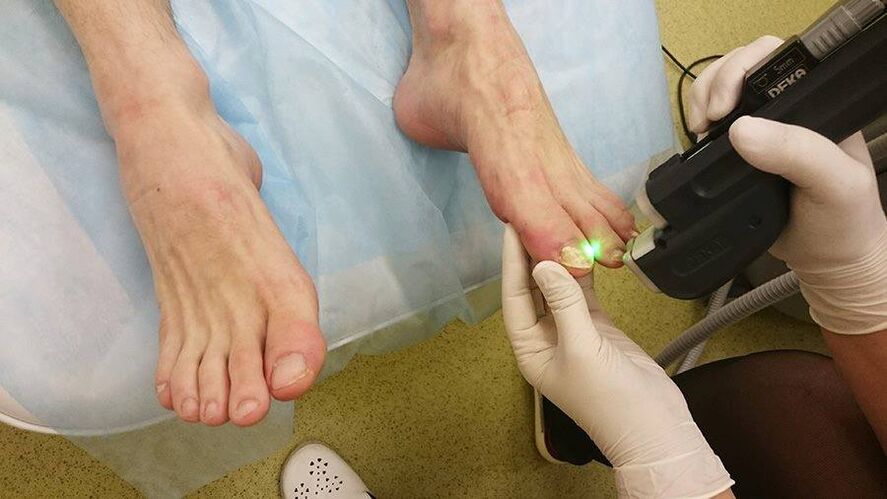
If the problem with nail fungus has noticeably worsened and any folk or official remedies practically do not give results, you can use an innovative solution - hardware treatment. This method is very effective and can be the only salvation in cases where other drugs are powerless.
Among the available techniques, laser treatment with an erbium laser is the most common. It cauterizes the mycelium and eliminates the visible symptoms of nail fungus. In addition, the technology allows you to clean the skin around the nails, between the toes and toes, restoring its former elasticity and attractiveness.
If you follow the basic rules of skin care for fungal diseases of the feet, it is quite possible to destroy this dangerous pathology. It is important not to delay treatment in the future and to immediately take appropriate action if questionable symptoms appear.















